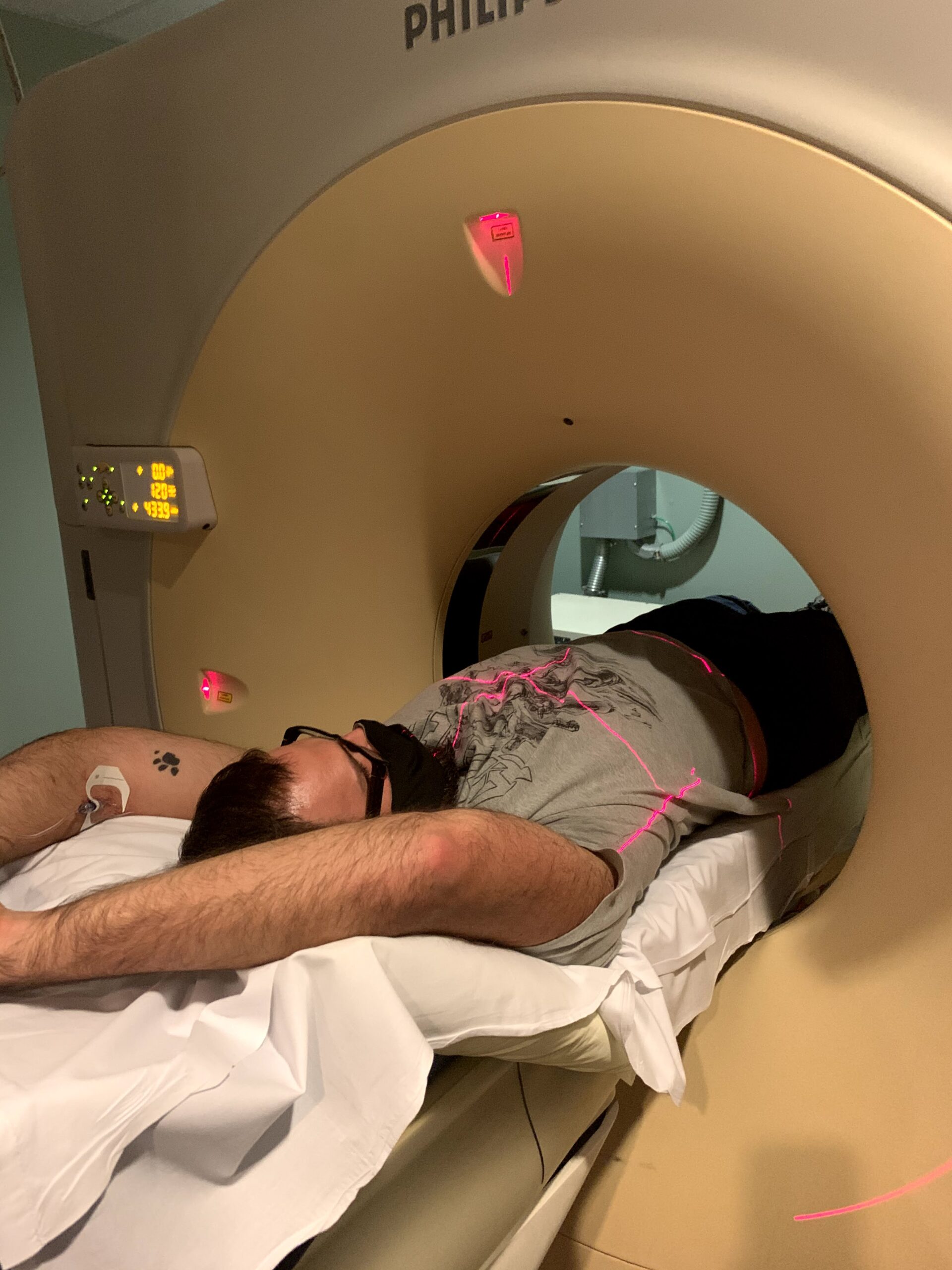
“Your X-Ray was Clear, Your Blood Work Showed No Markers for Testicular Cancer, and Your Orchiectomy Scar is Healing Well.”
On Friday, I had to go for my CT scan and X-Ray. These were to determine if the cancer had spread. The blood work they did showed no cancer markers, so Dr. Dumont seemed optimistic, but these were still necessary tests and would determine the next steps.
Overall, they were uneventful. I was given a wheelchair to help reduce pain in moving, which was a godsend. I had to get another IV put in for the contrast dye and the nurse who injected me was incredible. She said to breathe in and then breathe out hard right as she penetrated me with the needle. I felt almost no pain whatsoever. Where was she before my surgery?

When they were doing basic medical history questions, one of the nurses asked, “Have you ever been diagnosed with cancer?” to which I replied, “Yes, on Wednesday.” She was a little taken aback and apologized. I said there was no need for this, and she commented that I seemed to be taking it well. It all goes back to my mindset – I am going to get better, and being down about it won’t help.
I will fight and cope with happy thoughts.
This was also the first time I had left my house in a week. It was extremely exhausting and caused some pain. However, it was a nice break from the monotony of being cooped up all day.
The following morning, my mom went back to Pennsylvania and some friends came to visit. A cane I had ordered to help with mobility was delivered and gave me some more independence. Some of my old co-workers visited me over the weekend, but nothing else eventful happened. The pain was subsiding, but I still had some moments. It appeared things were slowly getting back to normal. Maybe this ordeal would be over soon.
Monday, November 7th brought forth the day of the post-op orchiectomy appointment.
It was a day that would prove to continue the trend of the worst of the possible two options becoming my reality.
“Your X-Ray was clear, your blood work showed no markers for cancer, and your scar looks to be healing really well. The numbness in your groin is normal; it will take a while for that to fully recover.”
Why wasn’t he mentioning the CT scan? With the exception of the X-Ray, I already knew everything he had just told me.
He took a deep breath and continued. “You CT scan showed enlarged lymph nodes. The cancer has spread.”
Triple wow. It was the third time a bombshell had dropped since this had all began. At this point, I kept expecting the worst. At first I knew a lump was concerning, and it was. I knew it was cancer before the biopsy came back. Of course it had spread; why would I get lucky at this point in the game?
“One of your lymph nodes was 2.1 centimeters, which isn’t the biggest they can be, but certainly big enough to be concerning.”
“How big are they usually?” I asked.
“Just a few millimeters. Usually they don’t show up on CT at all.” After teaching the metric system for three years, I knew that a few millimeters to 2.1 centimeters was a big deal. Who says school isn’t applicable to real life?
Dr. Dumont continued his diagnosis. “With testicular cancer, there are two types: Seminoma and nonseminoma. Your particular cancer falls under the latter category.”
Although, nonseminoma sounded like it was a good thing, something told me that I was wrong.
Dr. Dumont confirmed this.
“Nonseminoma (which is also called embryonal carcinoma) is more aggressive and spreads much more quickly. At this point, you are in Stage IIb cancer.”
Realistically, Stage IIb didn’t mean anything to me. All I had heard was that the cancer had spread. I wanted to know what was next.

“There are two options here. My recommendation is chemotherapy. The other option is major invasive surgery. They would remove your lymph nodes and biopsy those. You would have a scar from your chest to your groin.”
Now, that scar seems pretty cool. I would feel like The Rock in Walking Tall. However, I would also like to avoid being cut open. After further discussion, we found out that even after the surgery, I would most likely still need chemo. Dr. Dumont indicated that the surgery wasn’t a wise option.
Mallory reacted with emotion and tears, as was expected. Me? I was more or less numb. I know what needs to be done will be done. Grandpa’s mantra echoed in my head, “Just tell me what to do and I’ll do it.” My first instinct was to get my action steps nailed down now; process it later. It had been a whirlwind of a month, but the chaos had become my normalcy.
Now that testicular cancer was confirmed, I wanted more details on chemotherapy.
“So chemo,” I started, “What kind? Would it just be oral pills or would it – “
“You would need to go to an oncologist and receive it there. It’s recommended to complete 3-4 rounds.”
Another bombshell. This would mean more time off from the classroom. I know no one would blame me, but I would hold myself accountable for not being there for my students. I also knew this would mean having to tell my students and their families. That was a bridge I would need to cross, but I wasn’t ready to think about that yet.
The bombardment wasn’t quite done yet. “Before you start chemo, you should really bank some sperm, “ Dr. Dumont said. “The treatment sometimes will render you completely infertile. There is also about a 2% chance that we’ll have to remove the other testicle if it spreads.”
Mallory and I had discussed children here and there throughout the course of our relationship. We weren’t quite sure what we wanted, but to potentially have that option eliminated made me start thinking more seriously about it. I had just gotten over the shock of losing a testicle, and now my fertility was being threatened. More internal debates. More unanswered questions.
Dr. Dumont answered every question Mallory and I had. Waiting and seeing if anything changed would be a terrible idea, as would homeopathic remedies. I might lose my hair, I might get really sick from chemo, but I might not. The oncologist would be able to tell us more.
I needed to see an oncologist ASAP, but they were having lunch when the urology office called.
That amused me; the people would would be taking part of my virility and life from me were off having a delightful lunch. Lovely.
We also immediately started looking into banking some of my sperm. I quickly found out how expensive it was, but I had to think beyond the cost. We decided to bank some of my sperm the following morning, just in case.
“In most cases, this cancer is completely curable and that is a really good thing,” Dr. Dumont shared.
I was well aware of this fact. Dying from this was not something I was worried about, although it was something I had imagined as an improbable outcome. People had been reassuring me (or maybe themselves?) of this fact for the entire time. Knowing you are going to be cured doesn’t soften the blow when the immediate situation seems so dire.
I knew I had to update people.
Brian, my principal, for one, as this would mean more time off, especially because once the chemo was completed, I would need to be monitored every few months for the foreseeable future. I know he would never think it, but part of me wondered if he would regret hiring me. My friends and family were waiting with bated breath for results. Those who texted me received a terse reply from me, “It wasn’t good. We’ll talk more later.” Perhaps this wasn’t the best way to handle it, but I didn’t want to ignore them entirely. How Mallory felt was another area of concern to me, albeit a stupid area to concern myself with as I knew she was with me in sickness and in health. I was to be her husband, but with each appointment, my prognosis was getting worse and worse.
As had become the pattern, I had anticipated the worst and it came true. The physical pain from the surgery was improving each day, but the emotional pain was being exponentially compounded each time. I did my best to keep it in, but it was starting to show through. Keeping it in had always been my go-to. I know it’s not healthy, but it’s how I’ve managed.
“This isn’t a hereditary cancer nor are there environmental factors,” Dr. Dumont said as he ended my appointment.
“It’s just a bad luck cancer.”
Click here to read the next part of my story, in which I read up on homeopathic medicine.
A self exam is how most cases of testicular cancer are detected early. Click the image for video directions or click here for a larger version
Want to work with Justin? Click here to learn more.
ABSOT is endorsed by the Laughter Arts and Sciences Foundation, a registered 501.c.3 charity. To make a tax-deductible contribution to help continue ABSOT's work with testicular cancer awareness and men's health, click the image below.